I often see patients who are concerned about gluten sensitivity or celiac disease. Indeed, that is a common problem and many people do feel better if they removed processed foods, and gluten in particular, from their diet.
The problem is that it matters how you go about investigating your body's response to gluten.
What is celiac disease?
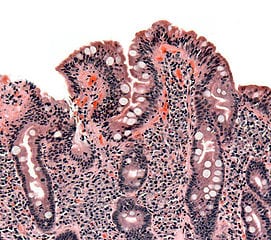
Celiac disease is an auto-immune response to gluten ingested in food. In other words, your own immune system attacks your body because it inappropriately reacts to gluten (contained in grains like wheat, rye and spelt) that you eat. Celiac disease can have all sorts of harmful effects on the body, ranging from diarrhea to anemia to nerve damage to increased rates of certain cancers.
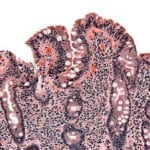
For more information on celiac disease, you can check out this article on UpToDate.com.
How can celiac disease be best diagnosed?
There is an important difference between gluten sensitivity and true celiac disease. Gluten sensitivity is more common, and can potentially be improved or reversed by improving the overall health of the intestinal mucosa and immune system. Celiac disease, however, tends to be a life-long problem and requires very strict removal of all gluten from the diet, forever. The consequences of not removing gluten strictly, if you have true celiac disease, can be increased risk of heart disease, cancer, and other serious illnesses down the line.
So I strongly recommend that everyone get properly tested, by a standard reference lab, for celiac disease before they remove gluten from their diet. If you do the tests after eliminating gluten, they often falsely come up normal, and you won't know. Again, you must be consuming some amount of gluten to get an accurate test result.
If you just have gluten sensitivity (diagnosed by an elimination-rechallenge experiment), there's hope that you can fix your intestinal permeability and no longer have to be perfect about gluten avoidance. However, if you have true celiac disease based on these tests, you must eliminate all gluten, strictly, for the rest of your life.
It's an important distinction.
What tests are most appropriate?
I usually recommend checking only a serum tissue transglutaminase IgA antibody (anti-tTG IgA) and a serum total immunoglobulin A (IgA) level. There are certain circumstances when other blood tests, and even endoscopic biopsies, are required, but most people can rely on these two simple tests. However, if the total IgA level is low, one must get further consultation to figure out how best to get an accurate test result.
How much do these tests cost?
Typically you will spend around $80-120 for the lab tests themselves, depending on where you go. Insurance may cover them if you have them done at a standard reference laboratory, ordered by a medical doctor, and have symptoms that “medically justify” the tests.
What if I've already eliminated gluten?
You have two choices. Continue off gluten very strictly, forever (i.e. assume you have true celiac disease). Or, you can restart eating some gluten daily for 4-6 weeks and then do the blood tests. It really can take that long to start making the antibodies again after you've eliminated gluten.
Where can I get these tests done?
Here in California, labs must be ordered by a licensed health care provider. So you'll need to visit a doctor who's willing to do this for you. Even better, one (like a doctor here at My Doctor Medical Group) who knows what things costs and who can get you fair and transparent pricing on the lab tests. You can also order these tests online from out-of-state companies, often at somewhat higher cost, without seeing a doctor.
What if I'm not sure what to do?
By all means, see a doctor who knows about these things, who can help explain your options and make sure you figure things out correctly. Like us, if you can come see us in San Francisco.







Comments 4
This article is pretty good to read. Excellent!!
Thank you very much for sharing, can I post it on my blog to share to my friends?
As long as you provide attribution and a link to the original post, sharing would be fine.
This article is pretty good to read. Excellent!!
Thank you very much for sharing, can I post it on my blog to share to my friends?
Author
As long as you provide attribution and a link to the original post, sharing would be fine.